I tend to keep my personal life well...personal, but there’s something about my personal life that I wanted to share with you with the hopes that it’ll bring more awareness to thinking about your own health.
You may have noticed an increasing trend and availability of gluten-free products and foods. Part of this growing trend is not because it’s hip and healthy to go gluten-free but because many individuals have discovered they actually have the autoimmune disorder Celiac Disease.
Recently, my girlfriend Lauren was diagnosed with Celiac Disease and she’s just one of the millions of people in the U.S. that are aware that they have the condition. In fact, Celiac advocacy groups estimate that as much as 75-83 percent of people with the disease are misdiagnosed or completely unaware because the disease often gets mistaken for something else or ignored altogether (Source).
There is no cure for Celiac. The only effective treatment is completely eliminating all traces of gluten from your diet.
Going without gluten isn’t the end of the world, but it definitely changes things about how she's going to eat. Many of her favorite foods contain gluten and she’ll now have to go without them for the rest of her life. Because she’s going gluten-free out of necessity, I’ll be going gluten-free out of support and I wanted to share our experience for a few reasons:
I wanted show my support for Lauren and the millions of other people that have Celiac Disease.
I wanted to raise your awareness about Celiac Disease. May is Celiac awareness month and in general, I want to encourage you to look into your health if you suspect something is wrong.
I wanted to share some insight into her diagnosis experience and how we're going to tackle going gluten-free. If you’re curious on how to reduce or eliminate gluten for your own reasons or perhaps, maybe you suspect or have Celiac, maybe our experience so far can help guide you through the process of going gluten-free.
Note: Please understand that I’m not a medical doctor. I’m only just sharing what we have experienced and learned so far in this journey. If you do suspect you have Celiac based on what I share here, you should definitely see your physician ASAP. Just make sure they listen.
Celiac Disease: A Brief Overview
Celiac is a chronic autoimmune disease that results in inflammation of the small intestine from ingesting gluten, a protein found in wheat, barley, rye and other cereal grains. In lay terms: it's basically a gluten allergy.
Source: BeyondCeliac.org
Your small intestine contains small, finger-like structures of tissue called villi. They are responsible for absorbing most of the nutrients from food after it’s been digested and broken down by your stomach. In Celiac patients, eating foods that contain gluten causes an immune response that causes your body’s own immune system to attack the small intestine. This attack damages the villi and prevents nutrients from being absorbed. This malabsorption causes a bunch of problems for the individual as you won’t have the building blocks to function healthily.
A diagram of what normal, healthy villi look like and function versus the villi of someone with Celiac (Source)
Celiac is genetic. If a parent, sibling or child in your family has Celiac, there’s a higher probability you may as well. The disease mostly affects women but can affect men as well. It can occur at any age and most people go years without knowing that they have the disease.
If left untreated and unmanaged, a bunch of bad things can happen to the gastrointestinal system and other complications can result over time like multiple sclerosis, osteoporosis, neurological disorders, infertility, certain cancers and an overall increase in mortality (source). Therefore, it’s important to recognize and be aware of the symptoms and get tested if you suspect something may be wrong.
The Signs of Celiac are Sneaky
Diagnosing Celiac is tricky. The problem is that symptoms of Celiac are pretty generic and very similar to other common ailments which are often just brushed off as “an angry tummy”. Lauren had no idea she was walking around with the disease and we still have no idea when it started.
According to some statistics, most people who have the disease don’t even know they have it. Sometimes it's mistaken for conditions like Irritable Bowel Syndrome (IBS). The classic symptom of Celiac is diarrhea (which is shared among a bunch of other conditions), but there can be a number of other symptoms present (or very few at all). For several months, Lauren experienced:
Bloating
Upset stomach
Painful stomach distention (she looked like she had a food baby 24/7)
Gas
Constipation (alternating with diarrhea)
Stomach Cramps
Rash/Itchy skin
Hair loss/hair thinning
Headaches
Brain fog
Anxiety
Fatigue
Source: BeyondCeliac.org
And they all just got worse over time.
The constant fatigue took it's toll the most. Lauren used to be an avid, competitive powerlifter who trained 5-6 days a week. Then gradually, she started to have less desire and energy to train or be active, regardless of how she ate or slept.
As time went on, she completely stopped training and stopped caring about lifting. Which deep down, I know that really bothered her not being able to do something she loved. She cried a lot more and was likely experiencing a bout of depression. The persistent abdominal pain and fatigue, seeing her body drastically run away from her, and the constant worry that something wasn’t right with her health made her increasingly more anxious and really started to wear her down mentally.
None of these things just appeared out of the blue. They gradually appeared and became more intense over the span of months until it was obvious that something wasn’t right. Remember with Celiac, you may have all of these symptoms, very few of them or they may be mild. So the only way you know for sure is to get tested.
What to do if you suspect Celiac (and why some doctors suck)
If you suspect you have Celiac, you can try to eliminate gluten from your diet for several weeks. If you start feeling better and then add it back and start feeling worse, there’s a decent chance gluten may be the culprit because as soon as a person with Celiac removes gluten, the gut will start repairing and healing. Unfortunately this means that if you remove gluten entirely by treating it like a food allergen, the removal means that doctors may not be able to accurately diagnose you. So if you want to know for sure, you have to continue to eat foods containing gluten.
Lauren’s first experience with the doctor didn’t fare well. Her first doctor spent very little time with her, didn’t ask her any questions about her symptoms or really listened at all. He didn’t even look up from his computer as he was taking notes or else he would have seen how miserable she was. He ordered some CT scans to rule out certain cancers and did some general blood work. Her imaging tests and blood work were interpreted as “normal” and the doctor told her she was fine, more than likely just had IBS and sent her on her way.
Knowing damn well there was something wrong, she got a second opinion.
Let that be a lesson: if you suspect and feel something is wrong with your body and you were giving a clear bill of health, ALWAYS get a second opinion!
The second doctor spotted some serious abnormalities in her original blood work and by this time, we were now very worried and fearing cancer. Thankfully, this doctor asked questions, listened and ordered the proper tests.
Doctors can detect Celiac with a blood test that looks for specific antibodies as long as you've been eating gluten (source). Her antibody test came back “98% positive” for Celiac. Although the test is pretty accurate, a false positive can sometimes register if you have other autoimmune disorders. In order to 100% confirm the blood tests, she then underwent an upper endoscopy procedure and had a biopsy of her small intestine. A biopsy is the only way to truly confirm and diagnose Celiac (source) and I wouldn't put too much stock getting an “at-home” test kit. If you really think you have a problem, you need to go see a doctor for testing.
Another lesson: You have to be very specific when you go to the doctor. If you suspect something like Celiac or any other autoimmune disease, communicate clearly with the doctor, do your research ahead of time, and ask for the proper tests! If the doctor dismisses you, find a new doctor! Trust your gut instinct. It's usually right.
How Do YOU Treat Celiac?
There is no cure for Celiac. The only effective treatment is completely eliminating all traces of gluten from your diet. This is probably just as stressful as having the disease itself.
Eliminating gluten is difficult because it’s literally everywhere. It’s not just in foods, but also in certain medicines, cosmetics like lipsticks, and even in kids’ play-doh. Unfortunately, even if a food is advertised as “gluten-free”, there is still a risk of cross-contamination from other gluten-containing products. Cross-contamination = just as bad as eating gluten straight up.
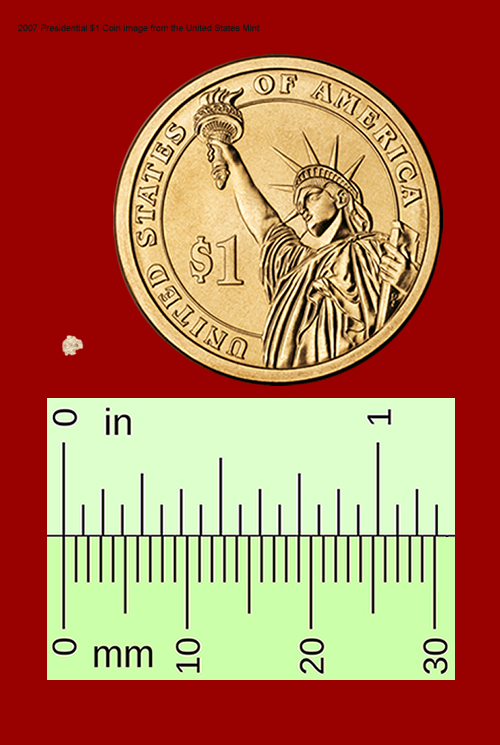
If you don’t have Celiac you can be a bit more relaxed about letting a little gluten slide into your diet but people with Celiac cannot tolerate even the tiniest amounts. Gluten in concentrations above 20 parts per million (ppm) will cause a reaction. If that’s hard for you to visualize, the amount of gluten in a breadcrumb the size of tip of a ball-point pen contains more than enough gluten to trigger the immune system to attack the gut.
The amount of gluten in this tiny crumb of bread is enough to cause a reaction and damage the intestine. Source: Wikipedia
A Crash Course in Going Gluten-Free
20 years or so ago, going gluten-free would have been much more difficult, but now with the abundance of gluten-free products, it’s a bit easier. There are still some things to be careful about and practice.
1. Completely avoid any foods containing gluten (duh)
Gluten is naturally found in products made from wheat, barley, rye, and triticale. This includes most:
Breads and baked goods (cakes, cornbread, pancakes, waffles, muffins, bagels, crackers, pies, cookies, brownies, pie crusts and etc)
Pastas and noodles (spaghetti, penne, fettucine, ramen, egg noodles, udon, and etc)
Breakfast cereals (even if they are made from corn they may have colorings or flavorings made from wheat. Also cross-contamination)
Any flour made from wheat, barley or rye
Flour Tortillas
Sauces (soy-sauce, gravies, or any sauces that use may wheat starch as a thickener. Be careful about sauced frozen veggies!)
Beer & beer yeast (some gluten-free beers exist. Check out my friends brewery Ginger's Revenge)
Certain chewing gums
Other cereal grains like oats may contain or be cross-contaminated with gluten since they are often handled in the same facilities. If you eat oatmeal, make sure it says “Gluten-free” on the box.
2. Stick to eating mostly whole, unprocessed foods.
You won’t really go wrong with eating fresh meats and fresh produce, and there are some grains and foods that are naturally gluten-free or are less likely to contain gluten. Foods that are generally safe for Celiac are:
Meats
Vegetables
Fruit
Fish & Seafoods
Nuts
Rice
Corn
Potato
Quinoa
Cassava
Beans & Legumes
Chia
Flax
Gluten-free oats (it must say gluten-free on the box)
That being said, be suspect of anything that comes in a package. Cross-contamination occurs frequently and only choose products that say "gluten-free" on the label.
3. Be consistent and very careful about checking food labels.
Most gluten-free foods have an icon or say “gluten-free” on the package. “Non-gluten containing foods/ingredients” doesn’t count as safe. In the U.S. “Gluten-free” is allowed on the package only when companies have properly tested the food and ingredients for gluten.
However, I pity the fool that trusts the label without looking at the ingredients! Food labeling isn’t well-regulated. For example, regulation allows for lumping hundreds of ingredients together as “Natural flavorings” (source).
Look for disclaimers that say something along the lines of “processed in a facility or on equipment that also processes wheat” or the allergen warning says “wheat”. If it says either of those things, it’s not safe.
Even though nuts are naturally gluten-free, you still need to check the label. If a food is processed on the same equipment as wheat, it's no bueno due to cross-contamination.
Always look carefully at the ingredients. Look for other names of gluten-containing foods including:
Wheat starch
Anything that says “wheat” (i.e. hydrolyzed wheat protein), barley or rye
Malt
Malt flavor
Malt extract
Malt vinegar
Triticale
Farina
Durum
Semolina
Bulgur
In addition, look for any red-flag ingredients that may contain gluten:
Dextrins
Dextrose
Natural or Artificial Colors
Modified starch
Really any starch
Stabilizers or binders
Emulsifiers
Flavorings
Baking Powder
If you see any of these double/triple check the ingredients and label for the words “gluten-free”.
If you’re in doubt about what’s in the food, don’t chance it and go without. If you’re questioning prescription medication, consult your doctor on what to do and call the drug manufacturer.
4. Home cook most of your meals
Gluten-free products and gluten-free dining are typically more expensive and could be cross-contaminated. So if you’re budget is tight and you want to avoid the gluten-belly, it’s better just to make your own food.
If you do go to a restaurant, you'll probably have to interrogate the hell out of the manager, server or kitchen staff to make sure things are gluten-free. If they offer gluten-free foods, make sure that you ask and confirm that gluten-free foods are kept separated from other foods containing gluten and they are prepared on dedicated surfaces or equipment. Tell them you have an allergy BEFORE you place an order. Otherwise, you run the risk of cross-contamination.
Even still, people and companies make mistakes. Your best bet is to prepare most if not all of your own meals.
5. You can still eat cookies and other bullshit on Gluten-free
Gluten-free doesn’t equal healthy. Sugar is gluten-free. We’ve actually managed to find a good niche of gluten-free ice cream, cookies, brownies, and other desserts. Some definitely taste like ass, but some are pretty damn good.
They definitely help with the transition and sting of going without a “real” slice of pizza or a cookie for the rest of life. However, gluten-free treats are still treats. They aren’t any healthier than their gluten-containing cousins. It’s still important to be conscious of how much of these foods you’re getting into your diet and limit them.
5. Focus on your gut health
Once you've cleared out gluten from your diet, your gut can start to heal. It's a good idea to take care of your gut to keep it happy and healthy long-term. Especially considering if you have Celiac, your gut biome is probably not in the best shape. To start optimizing your gut health:
Slowly ease into taking a probiotic. Start with a low dose about 5-10 Billion CFUs and work up to 25-30 Billion CFUs.
Add fermented foods to your diet and get enough fiber (30-40g a day)
Supplement with glutamine (work up to about 5g per day)
Drink bone broth or supplement with collagen peptides to help the gut lining recover
Supplement with Omega 3 fatty acids to help with inflammation
Manage stress and relax
7. You will probably mess up
It’s been about a week since we’ve gone completely gluten-free and we’ve already messed up. It’s going to happen and it’s ok. Just use each mess up as a learning lesson on what to avoid in the future. Good news is that having Celiac isn’t like a deathly peanut allergy. You won’t immediately die from it, but you’ll definitely know when you’ve messed up due to the onslaught of discomfort.
Keep a food journal or use a food app like to document when symptoms appear. Lauren uses an app called MySymptoms to document how foods make her fee and uses the app to look for any patterns or suspect foods.
Final thoughts
If you’re thinking you may have some issues with gluten, don’t ignore it. Autoimmune diseases are on the rise--especially Celiac and especially among women. Again, most people with Celiac don’t even know they have it. So if you suspect you may have a problem, go to the doctor! Take ownership of your health, exercise control of what you decide to put into your body, and take care of yourself.
If you have any questions for Lauren and I you can leave a comment or email me. Neither of us is a doctor, but we’re happy to share more about this experience so far. If you’re currently diagnosed with Celiac, we’d love to know how you handle the diet and lifestyle. Please reach out!
Thanks for reading.
Cheers,
Alex
References:
https://gluten.lovetoknow.com/How_Many_Celiacs_in_the_United_States
https://www.beyondceliac.org/celiac-disease/facts-and-figures/
https://celiac.org/celiac-disease/understanding-celiac-disease-2/what-is-celiac-disease/
Rubio-Tapia, Alberto et al. “Increased Prevalence and Mortality in Undiagnosed Celiac Disease.” Gastroenterology 137.1 (2009): 88–93. PMC. Web. 8 May 2018. (link)
Generally Recognized as Secret: Chemicals Added to Food in the United States. Tom Neltner, J.D. Maricel Maffini, Ph.D. Natural Resources Defense Council. NRDC report. April 2014 (link)
Interested in working with me?
I'm offering a free consult call for those want change their lives with better nutrition. To see how I can help you, click the button below to schedule your free 1-on-1 call.